A recent study found that ultrathin-strut Biodegradable Polymer Everolimus-Eluting Stents (BDP-EES) demonstrated safety and efficacy comparable to Durable Polymer Everolimus-Eluting Stents (DP-EES) over 24 months following Percutaneous Coronary Intervention (PCI). Clinical outcomes revealed nearly identical Major Adverse Cardiac Event (MACE) rates of 3.8% for the BDP-EES group compared to 3.7% for the DP-EES group. These findings were published in October 2025 in the Indian Heart Journal. The Evolution of Drug-Eluting Stent Technology: Drug-eluting stents (DES) have significantly lowered restenosis by utilizing polymer-based drug release, yet permanent polymers may delay arterial healing and increase risks of late complications. BDP-EES platforms were designed to mitigate these risks by degrading after the drug is eluted, potentially enhancing vascular recovery. Additionally, strut thickness is a critical performance factor; thinner struts, such as those in the ultrathin BDP-EES (65 μm), are intended to reduce vessel injury and improve deliverability compared to thicker platforms like the DP-EES (81 μm). Study Overview The retrospective, multicenter study was conducted across six Indian facilities, evaluating patients treated for Coronary Artery Disease (CAD). The analysis compared the Eternia stent (BDP-EES) against the Xience stent (DP-EES) over a 24-month clinical follow-up. Patients included those presenting with stable angina or acute coronary syndrome (ACS), which encompasses ST-segment elevation myocardial infarction (STEMI), non-ST-segment elevation myocardial infarction, and unstable angina. The study measured primary outcomes through a MACE composite, which includes cardiac death, myocardial infarction (MI), and target lesion revascularization (TLR). The key findings from the study include: • The MACE rates at 24 months were nearly identical between the BDP-EES (3.8%) and DP-EES (3.7%) groups, showing no statistically significant difference (p = 0.939). • Despite the comparable outcomes, patients receiving the BDP-EES were generally older and had a higher prevalence of complex chronic total occlusions (18.2% vs. 6.6%). • Safety profiles remained excellent, with no definite or probable Stent Thrombosis (ST) reported in either group, and possible thrombosis rates were minimal at 0.3% and 0.4%, respectively. Clinical Relevance and Long-term Performance For practicing cardiologists, this study confirms that the ultrathin-strut BDP-EES is a safe and effective alternative to established DP-EES platforms in routine clinical practice. The results highlight that even in a cohort with more complex lesions and older age, the biodegradable polymer technology maintained high safety standards and efficacy. While the performance was equivalent at 24 months, the theoretical benefit of polymer degradation may offer further long-term protection against late vascular events. Clinicians should note that the low rates of target vessel revascularization and stent thrombosis across both devices reinforce the reliability of modern stent designs. Overall, the choice of an ultrathin BDP-EES provides comparable clinical outcomes to the gold-standard DP-EES, supporting its use in diverse patient populations. Reference Kaul U, Garg PK, Chopra R, Gupta R, Mathur V. Ultra-low thickness bio-degradable polymer vs durable polymer everolimus eluting stents – A 24 months clinical follow-up study. Indian Heart Journal. 2025;77(6):467-470


Advanced Photon-Counting Computed Tomography (PCCT) has demonstrated a 100% diagnostic quality and revealed that 74% of asymptomatic patients with Coronary Artery Calcium (CAC) scores exceeding 1,000 Agatston Units (AU) do not possess severe coronary obstructive disease, as a recent study has shown. The study’s brief report was published in the Journal of the American College of Cardiology (JACC): Advances in February 2026. Bridging the Calcium Gap in Cardiac Imaging While extreme Coronary Artery Calcium (CAC) above 1,000 AU denotes significant cardiovascular risk, traditional Coronary Computed Tomography Angiography (CCTA) is frequently hampered by calcium-induced blooming artifacts; therefore, addressing this gap, the study aimed to evaluate whether the PCCT could reliably assess coronary stenosis in this difficult-to-image asymptomatic population. Study Overview The retrospective clinical evaluation conducted between February 2024 and March 2025 utilized a PCCT scanner at 0.2 mm slice thickness to evaluate 19 asymptomatic patients with extreme calcium burdens. Excluding those with prior cardiac events or revascularization, the researchers primarily sought to determine the diagnostic yield and the frequency of functionally significant disease via ultra-high-resolution imaging, using the Coronary Artery Disease–Reporting and Data System (CAD-RADS) 2.0 to categorize findings. Key Findings of the Study Include: Universal Clarity: Demonstrating that PCCT achieved 100% diagnostic quality across all segments, the study successfully bypassed the traditional blooming artifacts that typically obscure lumen assessment in high-calcium patients. Ischemia Exclusion: Confirming that all seven patients who underwent Fractional Flow Reserve derived from Computed Tomography (FFR-CT) had negative results between 0.80 and 0.93, the study suggests that most extreme calcium cases do not involve functionally significant blockages. Anatomic Insight: Categorizing the cohort, the research found that 32% of patients were classified as CAD-RADS 2 and 42% as CAD-RADS 3, providing a detailed map of nonobstructive disease distribution. Surgical Necessity: Identifying only one patient who required Coronary Artery Bypass Grafting (CABG) after Invasive Coronary Angiography (ICA) confirmed multivessel disease, the findings highlight PCCT’s ability to pinpoint the rare cases needing intervention. Reduced Testing: Observing that most participants required no further evaluation following their scan, the data underscores the potential of PCCT to limit redundant and invasive diagnostic procedures. Potential Clinical Implications For practicing physicians, PCCT provides a robust, noninvasive pathway to accurately risk-stratify asymptomatic patients with high calcium burdens, potentially sparing many from unnecessary invasive catheterization while precisely identifying those few who require surgical revascularization. Reference Shiyovich A, Blair CV, Aun JA, et al. Photon-Counting Coronary CT Angiography in Asymptomatic Patients With Extreme Coronary Artery Calcium Score. JACC Adv. 2026;5(2):102553.
A new research perspective was published in Volume 12 of Oncoscience on December 23, 2025, titled “Necrotizing fasciitis of the head and neck – clinical features, diagnostics, and management strategies.” Led by first author Anna Aydin, together with corresponding author Florian Dudde from the Army Hospital Hamburg, this expert perspective outlines key insights into the diagnosis and treatment of necrotizing fasciitis (NF) in the head and neck. It emphasizes the urgent need for early recognition, immediate surgery, and coordinated care to reduce the high mortality associated with this rare but fast-spreading infection. These recommendations are especially relevant for patients with cancer, diabetes, or weakened immune systems. Necrotizing fasciitis is a soft tissue infection that spreads rapidly and can cause severe illness or death within hours. Although it typically affects the limbs or abdomen, cases involving the head and neck are rare but especially dangerous due to their proximity to the airway and other vital structures. The perspective warns that early symptoms such as pain, swelling, and fever can be mild or misleading, which often leads to delays in diagnosis and treatment. In cancer patients, for example, symptoms may be mistaken for tumor-related changes or side effects of therapy. “A narrative review of the available literature was conducted and complemented by clinical experience from a tertiary referral center.” The authors highlight that contrast-enhanced CT scans are the most effective imaging tool for early diagnosis, as they help identify deep tissue damage and gas formation. Laboratory tools like the LRINEC score, often used to assess infection severity, are less reliable in head and neck cases and should not delay surgical action. The perspective reinforces that early and aggressive surgical removal of infected tissue, combined with broad-spectrum antibiotics and airway protection, is essential. Many patients require multiple surgeries and intensive care during the early stages of treatment. The role of hyperbaric oxygen therapy (HBOT) is also discussed. This treatment delivers high-pressure oxygen to fight infection and promote healing. While some studies suggest that HBOT may lower mortality and reduce the number of surgeries in certain patients, particularly those with anaerobic infections, the evidence is limited and inconsistent. Access to HBOT is also restricted to specialized centers, and delays in transfer may reduce its potential benefits. Despite medical advances, death rates for cervicofacial NF remain between 10% and 30%. Survivors often face long-term complications, including disfigurement, difficulty speaking or eating, and psychological distress. The authors call for more targeted research, especially for cancer patients, who may not present with typical symptoms. This expert perspective encourages clinicians to act quickly when NF is suspected and highlights the need for better diagnostic tools and treatment strategies. Raising awareness among oncologists, surgeons, and emergency care providers is essential to improve outcomes in this dangerous but often overlooked condition. Reference: Anna Aydin, Lawik Revend, Doha Revend, Oliver Schuck and Florian Dudde, Necrotizing fasciitis of the head and neck – clinical features, diagnostics, and management strategies, Oncoscience, https://doi.org/10.18632/oncoscience.639

Targeting a precise “Goldilocks zone” where low-density lipoprotein cholesterol (LDL-C) remains within 3.600 to 4.204 mmol/L and high-density lipoprotein cholesterol (HDL-C) stays between 1.421 and 1.699 mmol/L may be the definitive strategy for minimizing mortality and cardiovascular risk in the aging population, as a recent study has shown. The study was published in the Journal of the American College of Cardiology (JACC): Advances in February 2026. Addressing the Lipid Management Gap in Geriatrics While traditional guidelines advocate for aggressive cholesterol reduction, the foundational assumption that lower levels always equal better outcomes remains unproven in the elderly, creating a clinical gap in managing aging populations. To address this, the study aimed to evaluate the relationships of LDL-C and HDL-C with cardiovascular disease (CVD) risk in older adults. Study Overview The prospective cohort study utilized the U.K. Biobank (UKB) to monitor 150,798 participants aged 60 and older over a multi-year follow-up ending in 2022, employing multivariable Cox regression and restricted cubic splines (RCS) for data analysis. Investigators excluded individuals with pre-existing malignancies or baseline heart conditions to ensure a primary prevention focus, evaluating primary endpoints of incident disease and cardiovascular mortality across six percentile-stratified lipid subgroups. Key Findings of the Study Include: Study-identified Paradoxical LDL-C Risks: A U-shaped link revealed that low-density lipoprotein cholesterol levels below 2.211 mmol/L were associated with a 27% higher risk of cardiovascular death compared to the reference range. Research-validated HDL-C Complexity: Findings showed that high-density lipoprotein cholesterol displays an L-shaped curve for incident disease but a U-shaped mortality curve, with the highest concentrations over 2.174 mmol/L linked to a 26% increase in fatal cardiovascular events. Investigative Synergistic Hazard Escalation: When both lipid metrics deviated simultaneously from the optimal thresholds, participants experienced a 55% higher risk of developing new cardiovascular conditions. Cohort-confirmed Age Gradients: For every incremental rise in the risk tier, cardiovascular mortality increased by 12% in the younger-old group, significantly higher than the 7% rise seen in those aged 65 and older. Evidence-based Goldilocks Thresholds: Minimal risk was consistently observed within the “Goldilocks zone” of 3.600-4.204 mmol/L for LDL-C and 1.421-1.699 mmol/L for HDL-C. Potential Clinical Implications For practicing physicians, these results highlight the necessity of transitioning from a single-marker focus to integrated risk models that evaluate both lipid metrics simultaneously, as concurrent deviations from ideal ranges create a compounded risk for cardiovascular events. The data support moving away from uniform aggressive reduction strategies toward personalized, age-stratified approaches that maintain metabolic equilibrium and prevent the potential dangers of excessively low cholesterol levels in older populations. Reference Ye X, Du S, Chen S, et al. U-Shaped Lipid-CVD Links in Older Adults: Reversed LDL-C and HDL-C Associations and Goldilocks Zone. JACC Adv. 2026;5(2):102544.
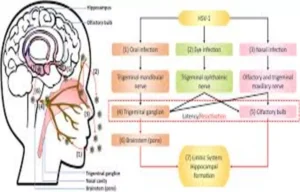
A new study published in JAMA has revealed that Valacyclovir did not improve cognitive outcomes and was associated with cognitive worsening in the primary outcome, indicating that it is not recommended for treating individuals with early symptomatic Alzheimer disease who are herpes simplex virus–seropositive. Neuroscientific, epidemiological, and electronic health record studies implicate herpes simplex virus (HSV) as potentially etiological for Alzheimer disease (AD). A study was done to compare the efficacy and adverse effects of valacyclovir vs placebo in participants with early symptomatic AD and HSV seropositivity (HSV-1 or HSV-2). This randomized clinical trial included adults with a clinical diagnosis of probable AD or a clinical diagnosis of mild cognitive impairment with positive biomarkers for AD, a positive serum antibody test (IgG or IgM) for HSV-1 or HSV-2, and a Mini-Mental State Examination score of 18 to 28. The trial was conducted at 3 US outpatient clinics specializing in memory disorders. Recruitment occurred from January 2018 to May 2022; the last follow-up occurred in September 2024. The primary outcome was least-squares mean (LSM) change at 78 weeks in the 11-item Alzheimer’s Disease Assessment Scale Cognitive (ADAS-Cognitive) Subscale score (range, 0-70; higher scores indicate greater impairment). The secondary outcomes were LSM change in the Alzheimer’s Disease Cooperative Study–Activities of Daily Living (ADCS-ADL) Scale score; LSM change in the 18F-florbetapir amyloid positron emission tomography (PET) standardized uptake value ratio (SUVR; higher scores indicate higher amyloid levels) for 6 brain regions (medial orbitofrontal, anterior cingulate, parietal lobe, posterior cingulate, temporal lobe, and precuneus); and LSM change in 18F-MK-6240 tau PET medial temporal SUVR (higher scores indicate higher tau levels) for 4 brain regions (amygdala, hippocampus, entorhinal, and parahippocampus). The frequency of adverse events was the safety outcome. Results Of the 120 participants (mean age, 71.4 [SD, 8.6] years; 55% were female), 93 (77.5%) completed the trial. At 78 weeks, the LSM change in the 11-item ADAS-Cognitive Subscale score was 10.86 (95% CI, 8.80 to 12.91) in the valacyclovir group vs 6.92 (95% CI, 4.88 to 8.97) in the placebo group, indicating greater cognitive worsening with valacyclovir than placebo (between-group difference, 3.93 [95% CI, 1.03 to 6.83]; P = .01). The LSM change in the ADCS-ADL Scale score at 78 weeks was −13.78 (95% CI, −17.00 to −10.56) in the valacyclovir group vs −10.16 (95% CI, −13.37 to −6.96) in the placebo group (between-group difference, −3.62 [95% CI, −8.16 to 0.93]). At 78 weeks, the LSM change in the 18F-florbetapir amyloid PET SUVR was 0.03 (95% CI, −0.04 to 0.10) in the valacyclovir group vs 0.01 (95% CI, −0.06 to 0.08) in the placebo group (between-group difference, 0.02 [95% CI, −0.08 to 0.12]). The LSM change in the 18F-MK-6240 tau PET medial temporal SUVR at 78 weeks was 0.07 (95% CI, −0.06 to 0.19) in the valacyclovir group vs −0.04 (95% CI, −0.15 to 0.07) in the placebo group (between-group difference, 0.11 [95% CI, −0.06 to 0.28]). The most common adverse events were elevated serum creatinine level (5 participants [8.3%] in the valacyclovir group vs 2 participants [3.3%] in the placebo group) and COVID-19 infection (3 [5%] vs 2 [3.3%], respectively). Valacyclovir was not efficacious with cognitive worsening for the primary outcome and it is not recommended to treat individuals with early symptomatic AD and HSV seropositivity. Reference: Devanand DP, Wisniewski T, Razlighi Q, et al. Valacyclovir Treatment of Early Symptomatic Alzheimer Disease: The VALAD Randomized Clinical Trial. JAMA. 2026;335(6):511–522. doi:10.1001/jama.2025.21738 Keywords: Cognitive, Worsening, Absence, Benefit, HSV-Seropositive, Early, Alzheimer, Disease, JAMA, Devanand DP, Wisniewski T, Razlighi