Switzerland: Adults with type 1 diabetes using CGM and a smart insulin pen achieved higher time in range when they consistently gave bolus insulin after missed-dose or high-glucose alerts. Faster responses to these alerts were strongly linked to improved glucose control.
The new real-world analysis published in Diabetic Medicine provides fresh insights into how people with type 1 diabetes can optimize outcomes using the Smart Multiple Daily Insulin (MDI) system. Led by Ohad Cohen and colleagues from Medtronic Diabetes, the study evaluated data from 1,852 adults across 21 countries, aiming to understand how user interactions with the system influence glycaemic targets.
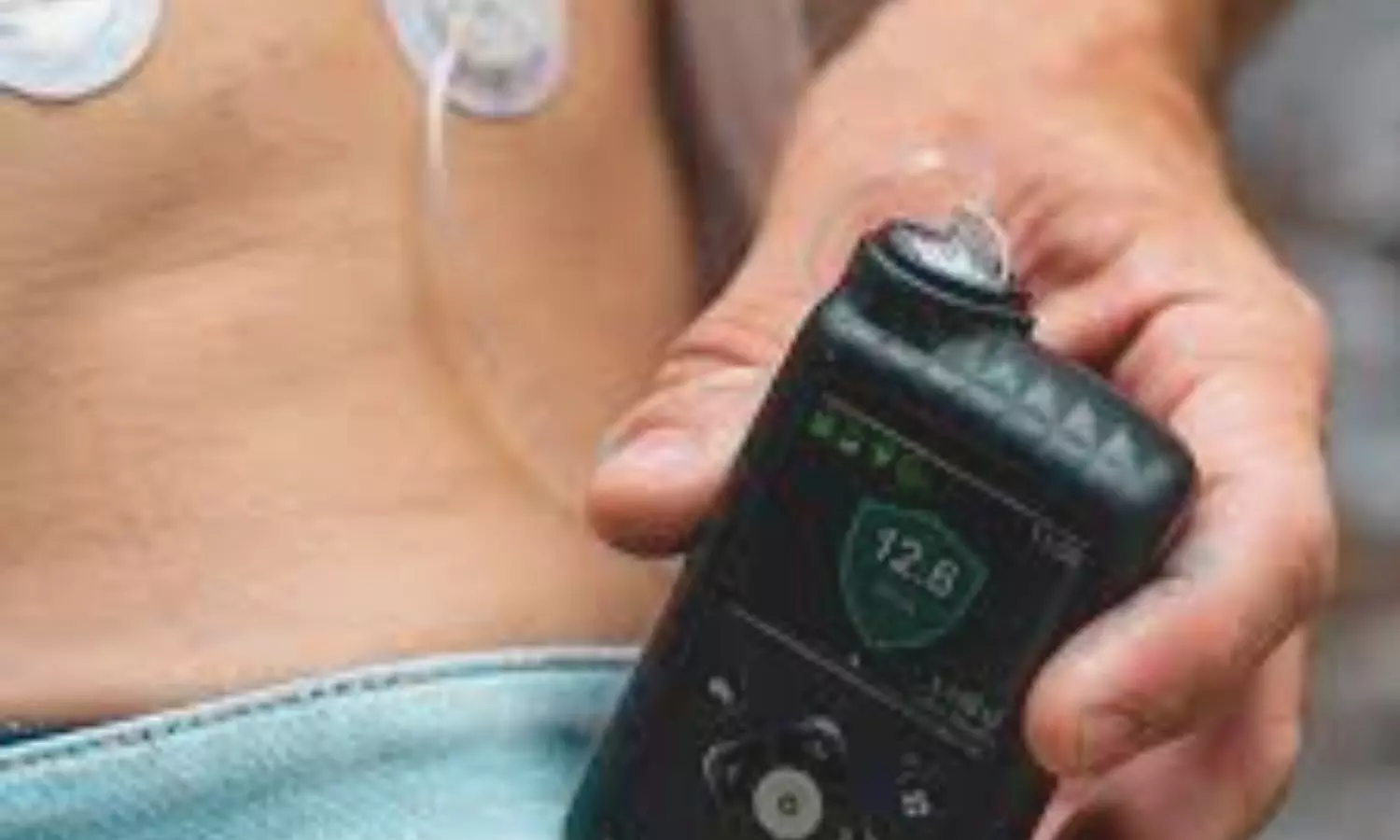
The Smart MDI ecosystem—comprising the InPen insulin injector, Simplera CGM, and the InPen mobile app—offers actionable alerts for missed bolus doses and high glucose levels. To be included in the analysis, participants needed at least 10 days of both InPen and CGM data. Researchers then examined how timely and consistent responses to missed-dose alerts (MDA) and correct high-glucose alerts (CHGA) affected glucose control.
Key Findings:
- The average time in range (TIR) across the cohort was 55.7%.
- Users responded to 49.3% of missed-dose alerts and 46.6% of high-glucose alerts with a corrective insulin bolus.
- Participants who responded to at least 75% of alerts within one hour achieved higher TIRs of 67.2% for missed-dose alerts and 71.5% for high-glucose alerts.
- Users who delivered a bolus within 10 minutes of an alert reached even higher TIRs of 68.6% and 71.9%, respectively.
- Increased responsiveness did not raise the risk of hypoglycaemia, with all groups staying well below the recommended time-below-range threshold.
- Nearly one-fourth of users met international CGM goals of more than 70% TIR and below 7% GMI.
- Among those who responded to over 75% of missed-dose alerts, the proportion meeting both targets almost doubled.
- More than half of users who quickly addressed high-glucose alerts achieved both glycaemic targets, reinforcing the link between prompt alert responses and improved glucose stability.
Researchers noted that the difference in TIR between highly responsive and less responsive users was largely explained by time spent in the tighter 70–140 mg/dL glucose range. This suggests that quick action on alerts directly contributes to maintaining normoglycaemia.
Although the cross-sectional design prevents proving causality, the consistent patterns suggest clear benefits from proactive user engagement. The study also emphasized the need for structured education, with experts already advocating guided training for clinicians and users to ensure actionable alerts lead to effective decisions. The authors noted that, unlike automated insulin delivery systems, the Smart MDI system depends heavily on user input, making education even more essential.
Limitations included reliance on self-reported demographic data, lack of baseline pre-system glycaemic information, and potential gaps in manually entered insulin doses. Even so, clear trends emerged, offering valuable real-world evidence from early users across Europe, the Middle East, and Africa.
The authors call for longitudinal follow-up to better understand long-term behaviour patterns, adherence, and the potential need for therapy adjustments. For now, the message is clear: consistent, timely reactions to Smart MDI alerts can significantly boost glucose outcomes for people living with type 1 diabetes.
Reference:
Laurenzi, A., Edd, S. N., Adolfsson, P., Piazza, F. D., Voelker, B., Im, G., & Cohen, O. (2025). Insights into the effective use of the Smart MDI system: Data from the first 1852 type 1 diabetes users. Diabetic Medicine, 42(12), e70161. https://doi.org/10.1111/dme.70161