USA: A secondary analysis of a randomized trial of preterm infants on continuous positive airway pressure (CPAP) has found that early caffeine administration combined with less invasive surfactant administration (LISA) did not lower the risk of death or moderate-to-severe neurodevelopmental impairment (NDI) based on Bayley Scales of Infant Development (BSID) assessment at two years. However, infants treated with LISA were more likely to achieve fine motor scores within the normal range on the Ages and Stages Questionnaire (ASQ-3) developmental screening.
Published in JAMA Network Open, the study led by Dr. Rebecca A. Dorner and colleagues evaluated whether early caffeine plus LISA improves long-term neurodevelopmental and respiratory outcomes in extremely preterm infants.
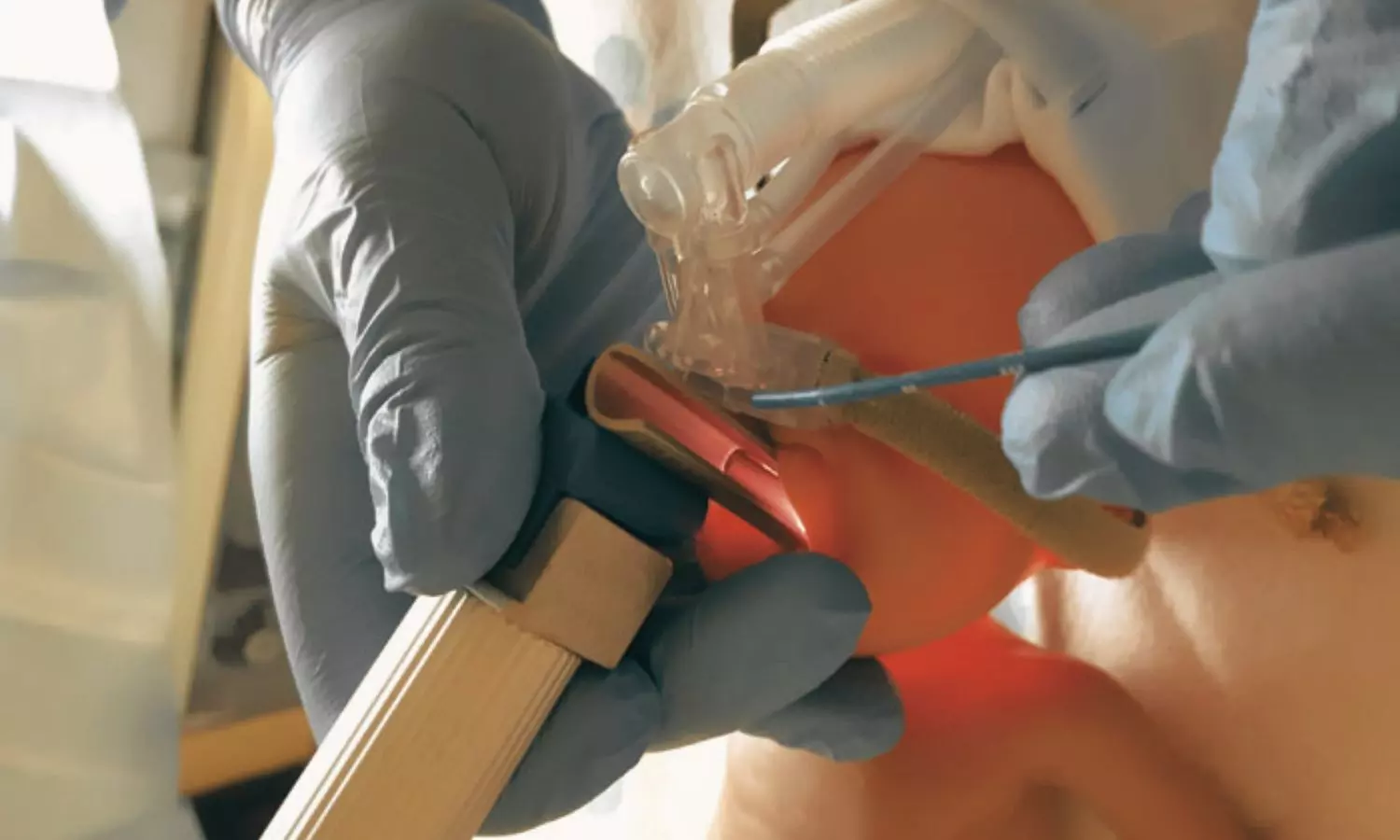
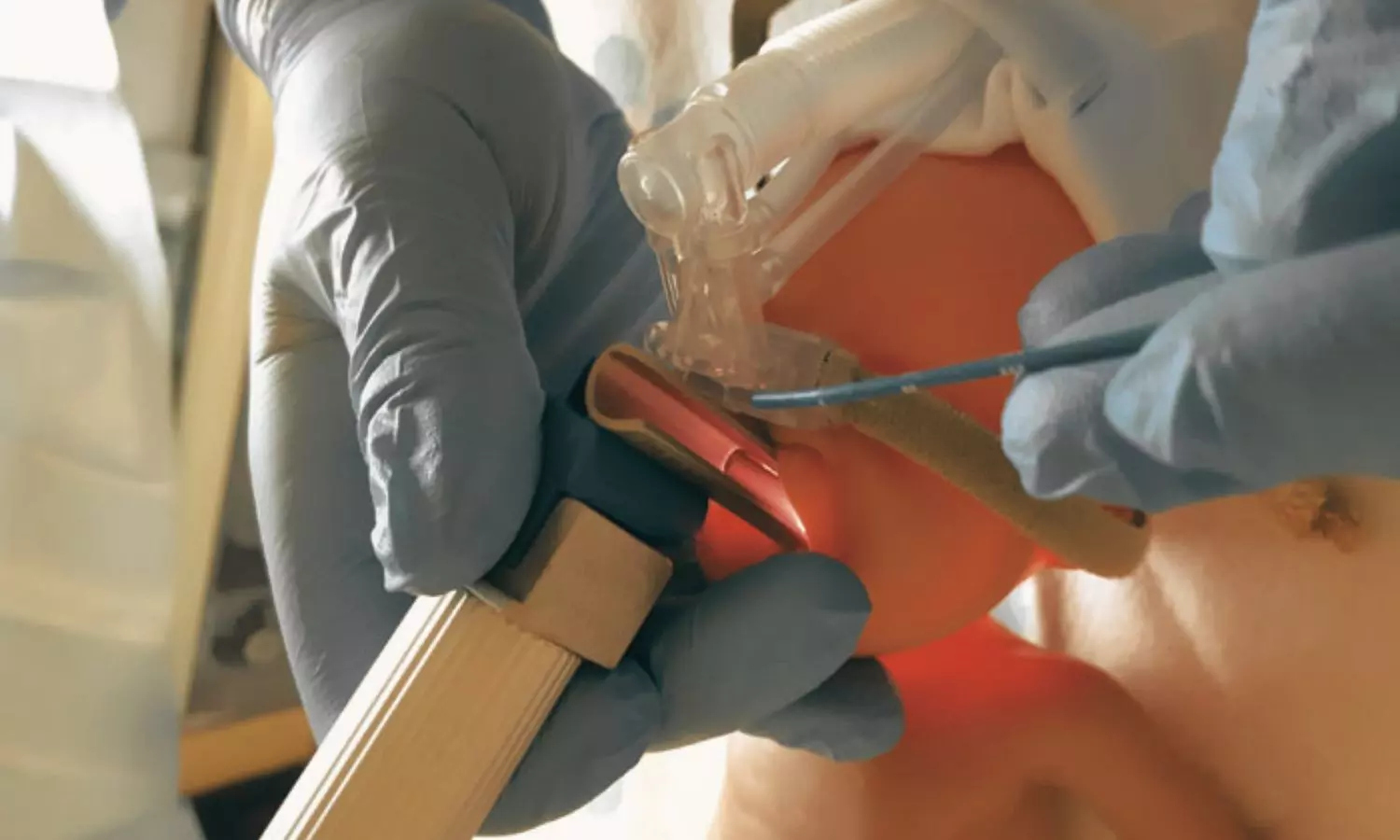
LISA is increasingly used to minimize the need for endotracheal intubation in preterm neonates with respiratory distress, though its long-term developmental impact remains unclear.
For this purpose, the researchers conducted a prespecified secondary analysis of a randomized trial including infants born between 24 weeks and 29 weeks 6 days of gestation across three academic centers in California, with follow-up from May 2022 to April 2025. Infants received intravenous caffeine within two hours of birth and were assigned to LISA or CPAP alone.
Of the 180 randomized infants, 147 (over 80%) had two-year follow-up data. The primary outcome was a composite of death or moderate-to-severe NDI at corrected age of two years, assessed using BSID. Secondary outcomes included ASQ-3 developmental screening and postdischarge respiratory outcomes such as medication use and hospitalizations.
The following were the key findings;
- Death or moderate-to-severe neurodevelopmental impairment occurred in 23% of infants in the LISA group compared to nearly 33% in the CPAP-only group.
- The observed difference between the groups was not statistically significant.
- No significant differences were found in overall developmental categories between the two groups.
- Rates of potential developmental delay on ASQ-3 screening were comparable across both groups.
- Infants receiving LISA showed better fine motor outcomes.
- A higher proportion of infants in the LISA group achieved fine motor scores within the expected range.
- No differences were noted in respiratory outcomes between the groups.
- Use of bronchodilators and corticosteroids was similar in both groups.
- Rates of hospital readmissions due to respiratory illness did not differ between the groups.
The authors concluded that while LISA combined with early caffeine does not appear to significantly reduce the risk of death or major neurodevelopmental impairment at two years, it may offer modest benefits in specific developmental domains such as fine motor skills. They emphasized the need for further research to better understand the long-term implications of less invasive respiratory interventions in this vulnerable population.
Reference:
Dorner RA, Morales A, Banerji A, et al. Two-Year Outcomes of Less Invasive Surfactant Administration Among Preterm Neonates: A Secondary Analysis of a Randomized Clinical Trial. JAMA Netw Open. 2026;9(3):e263852. doi:10.1001/jamanetworkopen.2026.3852