China: In a recent case report published in BMC Nephrology, Yaqing Liu and colleagues from the Department of Pediatrics at the First Affiliated Hospital of Gannan Medical University, China, document a unique clinical presentation combining Peutz-Jeghers syndrome (PJS) and unilateral multicystic dysplastic kidney (MCDK) in a teenage girl. This unusual co-occurrence not only sheds light on a possible novel function of the STK11 gene but also opens the door to new perspectives on congenital kidney anomalies in the context of genetic syndromes.
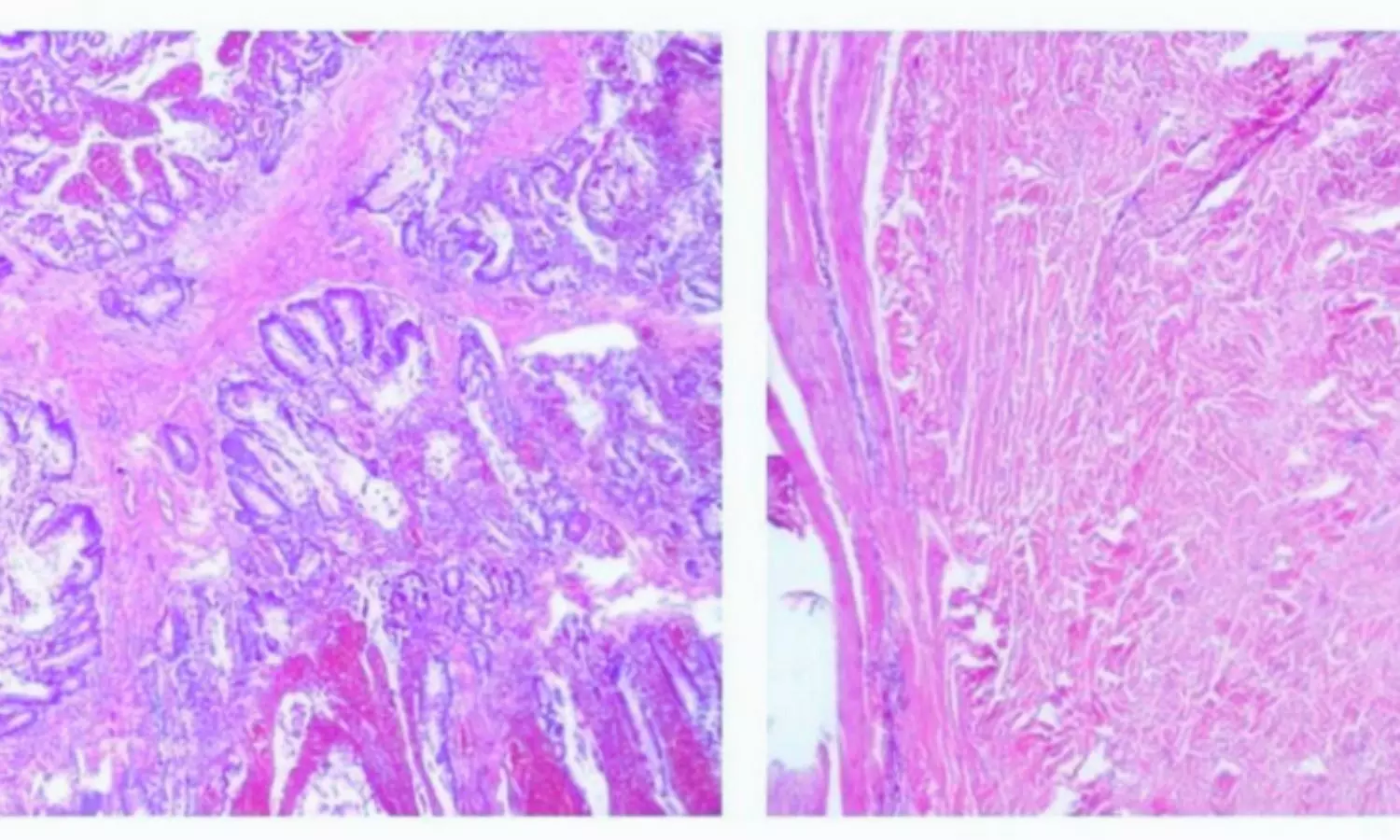
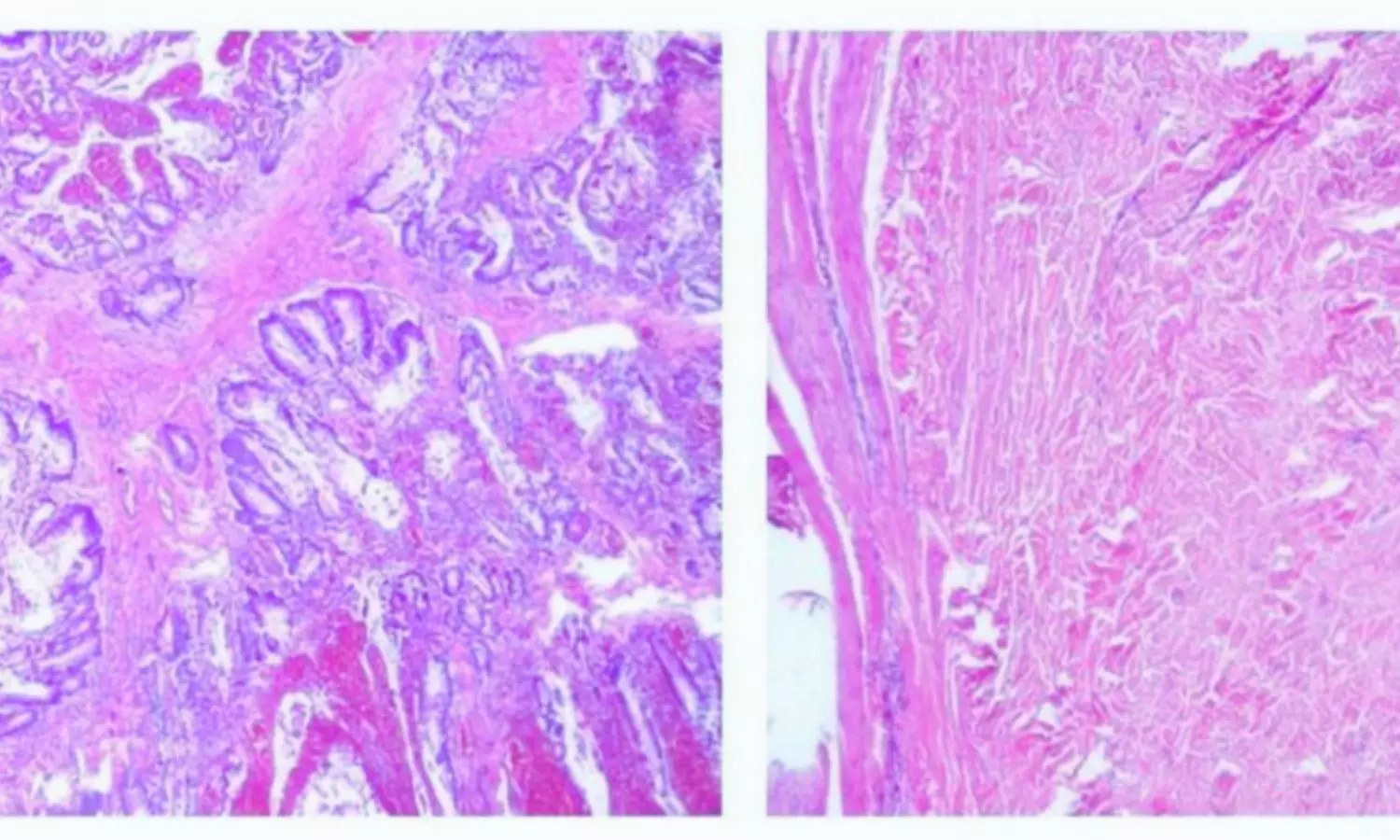
The case involved a 13-year-and-7-month-old girl who presented with abdominal pain and a history of gastrointestinal issues, including intussusception and multiple polyps—hallmarks of PJS. Additionally, dark pigmented spots on her lips and fingers supported the diagnosis. Genetic analysis revealed a de novo pathogenic mutation in the STK11 gene—specifically, a c.843del frameshift variant—confirming the diagnosis of Peutz-Jeghers syndrome.
However, what makes this case particularly noteworthy is the simultaneous presence of MCDK, a rare kidney malformation. Although initially misdiagnosed as right kidney agenesis during childhood, further imaging revealed a severely underdeveloped right kidney with multiple cystic lesions and compensatory hypertrophy of the left kidney. These findings challenge the traditional understanding of STK11 mutations as purely cancer-related and suggest their potential involvement in kidney development.
The patient underwent multiple surgeries, including laparoscopic reduction of intestinal intussusception and partial small bowel resections, due to persistent symptoms and postoperative complications. Despite these challenges, her condition stabilized following discharge, and she experienced significant improvement, including a 10-kilogram weight gain within six months and the onset of regular menstruation.
From a research standpoint, this case proposes three possible molecular mechanisms linking STK11 to kidney development: disrupted metabolic signaling during organogenesis, a ciliopathy-like disease pathway, and altered epigenetic regulation affecting developmental plasticity. These hypotheses invite future investigation into the broader role of STK11 beyond tumor suppression.
Liu and her team emphasize the importance of systematic renal evaluation in patients diagnosed with Peutz-Jeghers syndrome, even in the absence of urinary symptoms. While this case may represent a rare occurrence, it signals a potential shift in how clinicians screen and manage PJS patients, particularly concerning congenital anomalies.
Nevertheless, the authors acknowledge several limitations. The dysplastic kidney was not surgically removed, preventing histopathological confirmation, and the follow-up period was relatively short. Moreover, without additional documented cases, a definitive genetic link between PJS and MCDK remains speculative. Still, this report provides a compelling foundation for further research into the developmental implications of STK11 mutations.
“Ultimately, the case highlights the need for heightened clinical awareness and interdisciplinary collaboration when addressing rare coexisting conditions, especially those involving genetic and congenital components,” the authors concluded.
Reference:
Liu, Y., Hu, S., Gan, Y. et al. Co-occurrence of Peutz-Jeghers syndrome and unilateral multicystic dysplastic kidney: a case report. BMC Nephrol 26, 396 (2025). https://doi.org/10.1186/s12882-025-04340-8